4.4 Special Warnings and Precautions for use
Montelukast
Acute Asthma: Montelukast is not indicated for use in the reversal of bronchospasm in acute asthma attacks, including status asthmaticus. Patients should be advised to have appropriate rescue medication available. Therapy with montelukast can be continued during acute exacerbations of asthma. There are no data demonstrating that oral corticosteroids can be reduced when montelukast is given concomitantly.
Patients who have exacerbations of asthma after exercise should have available for rescue a short-acting inhaled beta2-agonist.
Concomitant Corticosteroid Use: While the dose of inhaled corticosteroid may be reduced gradually under medical supervision, montelukast should not be abruptly substituted for inhaled or oral corticosteroids.
Aspirin Sensitivity: Patients with known aspirin sensitivity should continue avoidance of aspirin or non-steroidal anti-inflammatory agents while taking montelukast. Although montelukast is effective in improving airway function in asthmatics with documented aspirin sensitivity, it has not been shown to truncate bronchoconstrictor response to aspirin and other non-steroidal anti-inflammatory drugs in aspirin-sensitive asthmatic patients.
Eosinophilic Conditions: Patients on therapy with montelukast may present with systemic eosinophilia sometimes presenting with clinical features of vasculitis consistent with Churg-Strauss syndrome, a condition, which is often treated with systemic corticosteroid therapy. These events usually, but not always, have been associated with the reduction of oral corticosteroid therapy. Physicians should be alert to eosinophilia, vasculitic rash, worsening pulmonary symptoms, cardiac complications, and/or neuropathy presenting in their patients. A causal association between, montelukast and these underlying conditions has not been established.
Neuropsychiatric Events: Neuropsychiatric events have been reported in adult, adolescent, and pediatric patients taking montelukast. Post-marketing reports with montelukast use include agitation, aggressive behavior or hostility, anxiousness, depression, disorientation, obsessive-compulsive symptoms, dream abnormalities, hallucinations, insomnia, irritability, memory impairment, restlessness, somnambulism, suicidal thinking and behavior (including suicide), and tremor. The clinical details of some post-marketing reports involving montelukast appear consistent with a drug-induced effect.
Patients and prescribers should be alert for neuropsychiatric events. Patients should be instructed to notify their prescriber if these changes occur. Prescribers should carefully evaluate the risks and benefits of continuing treatment with montelukast if such events occur.
Levocetirizine
Somnolence: In clinical trials the occurrence of somnolence, fatigue, and asthenia has been reported in some patients under therapy with RHINAM. Patients should be cautioned against engaging in hazardous occupations requiring complete mental alertness, and motor coordination such as operating machinery or driving a motor vehicle after ingestion of RHINAM. Concurrent use of RHINAM with alcohol or other central nervous system depressants should be avoided because additional reductions in alertness and additional impairment of central nervous system performance may occur.
Urinary Retention: Urinary retention has been reported post marketing with RHINAM. RHINAM should be used with caution in patients with predisposing factors of urinary retention (e.g. spinal cord lesion, prostatic hyperplasia) as RHINAM may increase the risk of urinary retention. Discontinue RHINAM if urinary retention occurs.
4.5 Drug Interactions
Montelukast
Montelukast may be administered with other therapies routinely used in the prophylaxis and chronic treatment of asthma. In drug-interaction studies, the recommended clinical dose of montelukast did not have clinically important effects on the pharmacokinetics of the following medicinal drugs: theophylline, prednisone, prednisolone, oral contraceptives (norethindrone 1 mg/ethinyl estradiol 35 mcg), terfenadine, digoxin and warfarin, gemfibrozil, itraconazole, thyroid hormones, sedative hypnotics, non-steroidal anti-inflammatory agents, benzodiazepines, decongestants, and CYP 450 enzyme inducers.
The area under the plasma concentration curve (AUC) for montelukast was decreased approximately 40% in subjects with co-administration of phenobarbital. Since montelukast is metabolised by CYP 3A4, 2C8 and 2C9, caution should be exercised, particularly in children, when montelukast is co-administered with inducers of CYP 3A4, 2C8 and 2C9 such as phenytoin, phenobarbital and rifampicin.
In vitro studies have shown that montelukast is a potent inhibitor of CYP 2C8. However, data from a clinical drug-drug interaction study involving montelukast and rosiglitazone (a probe substrate representative of medicinal products primarily metabolised by CYP 2C8) demonstrated that montelukast does not inhibit CYP 2C8 in vivo. Therefore, montelukast is not anticipated to markedly alter the metabolism of medicinal products metabolised by this enzyme (e.g., paclitaxel, rosiglitazone, and repaglinide.)
In vitro studies have shown that montelukast is a substrate of CYP 2C8, and to a less significant extent, of 2C9, and 3A4. In a clinical drug-drug interaction study involving montelukast and gemfibrozil (an inhibitor of both CYP 2C8 and 2C9) gemfibrozil increased the systemic exposure of montelukast by 4.4-fold. No routine dosage adjustment of montelukast is required upon co-administration with gemfibrozil or other potent inhibitors of CYP 2C8, but the physician should be aware of the potential for an increase in adverse reactions.
Based on in vitro data, clinically important drug interactions with less potent inhibitors of CYP 2C8 (e.g., trimethoprim) are not anticipated. Co-administration of montelukast with itraconazole, a strong inhibitor of CYP 3A4, resulted in no significant increase in the systemic exposure of montelukast.
Levocetirizine
In vitro data indicate that levocetirizine is unlikely to produce pharmacokinetic interactions through inhibition or induction of liver drug-metabolizing enzymes. No in vivo drug-drug interaction studies have been performed with levocetirizine. Drug interaction studies have been performed with racemic cetirizine.
Antipyrine, Azithromycin, Cimetidine, Erythromycin, Ketoconazole, Theophylline, and Pseudoephedrine: Pharmacokinetic interaction studies performed with racemic cetirizine demonstrated that cetirizine did not interact with antipyrine, pseudoephedrine, erythromycin, azithromycin, ketoconazole, and cimetidine. There was a small decrease (~16%) in the clearance of cetirizine caused by a 400 mg dose of theophylline. It is possible that higher theophylline doses could have a greater effect.
Ritonavir: Ritonavir increased the plasma AUC of cetirizine by about 42% accompanied by an increase in half-life (53%) and a decrease in clearance (29%) of cetirizine. The disposition of ritonavir was not altered by concomitant cetirizine administration.
4.6 Use in special populations
Patients with Renal Impairment
Montelukast: No dosage adjustment is recommended for montelukast in patients with renal impairment.
Levocetirizine: Levocetirizine is known to be substantially excreted by the kidneys and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Dosage adjustment may be required in patients with impaired renal function. Hence this combination is not recommended in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection and it may be useful to monitor renal function.
Patients with Hepatic Impairment
Montelukast: No dosage adjustment is required in patients with mild-to-moderate hepatic insufficiency. The pharmacokinetics of montelukast in patients with more severe hepatic impairment or with hepatitis have not been evaluated.
Levocetirizine: As levocetirizine is mainly excreted unchanged by the kidneys, it is unlikely that the clearance of levocetirizine is significantly decreased in patients with solely hepatic impairment.
Pregnant Women
There are no adequate and well controlled studies of either montelukast or levocetirizine in pregnant women. Animal studies do not indicate harmful effects with respect to effects on pregnancy or embryonal/foetal development.
Montelukast: Animal studies do not indicate harmful effects with respect to effects on pregnancy or embryonal/foetal development. Limited data from available pregnancy databases do not suggest a causal relationship between Montelukast and malformations (i.e. limb defects) that have been rarely reported in worldwide post marketing experience. Montelukast may be used during pregnancy only if it is considered to be clearly essential.
Levocetirizine: There are no or limited amount of data (less than 300 pregnancy outcomes) from the use of levocetirizine in pregnant women. However, for cetirizine, the racemate of levocetirizine, a large amount of data (more than 1000 pregnancy outcomes) on pregnant women indicate no malformative or feto/neonatal toxicity. Animal studies do not indicate direct or indirect harmful effects with respect to pregnancy, embryo/fetal development, parturition or postnatal development. The use of levocetirizine may be considered during pregnancy, if necessary. Because animal reproduction studies are not always predictive of human response, this combination should be used during pregnancy only if it is considered to be clearly essential.
Lactating Women
Montelukast: Studies in rats have shown that montelukast is excreted in milk. It is not known if montelukast is excreted in human milk. Montelukast may be used in breast-feeding mothers only if it is considered to be clearly essential.
Levocetirizine: No peri and postnatal animal studies have been conducted with levocetirizine. Cetirizine has been reported to be excreted in human breast milk. Because levocetirizine is also expected to be excreted in human milk this combination is not recommended during lactation.
Pediatric Patients
Montelukast: Safety and efficacy of montelukast have been established in adequate and well-controlled studies in pediatric patients with asthma 6 to 14 years of age. Safety and efficacy profiles in this age group are similar to those seen in adults. The efficacy of montelukast for the treatment of seasonal allergic rhinitis in pediatric patients 2 to 14 years of age and for the treatment of perennial allergic rhinitis in pediatric patients 6 months to 14 years of age is supported by extrapolation from the demonstrated efficacy in patients 15 years of age and older with allergic rhinitis as well as the assumption that the disease course, pathophysiology and the drug's effect are substantially similar among these populations.
Levocetirizine: The recommended dose of levocetirizine for the treatment of the uncomplicated skin manifestations of chronic idiopathic urticaria in patients 6 months to 17 years of age is based on extrapolation of efficacy from adults 18 years of age and older. The recommended dose of levocetirizine in patients 6 months to 2 years of age for the treatment of the symptoms of perennial allergic rhinitis and 6 months to 11 years of age with chronic idiopathic urticaria is based on cross-study comparisons of the systemic exposure of levocetirizine in adults and pediatric patients and on the safety profile of levocetirizine in both adult and pediatric patients at doses equal to or higher than the recommended dose for patients 6 months to 11 years of age.
Geriatric Patients
Montelukast: Of the total number of subjects in clinical studies of montelukast, 3.5% were 65 years of age and over, and 0.4% were 75 years of age and over. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and younger patients, but greater sensitivity of some older individuals cannot be ruled out. The pharmacokinetic profile and the oral bioavailability of a single 10-mg oral dose of montelukast are similar in elderly and younger adults. The plasma half-life of montelukast is slightly longer in the elderly. No dosage adjustment in the elderly is required.
Levocetirizine: Clinical studies of levocetirizine for each approved indication did not include sufficient numbers of patients aged 65 years and older to determine whether they respond differently than younger patients. Other reported clinical experience has not identified differences in responses between the elderly and younger patients. In general, dose selection for an elderly patient should be cautious usually starting at the low end of the dosing range reflecting the greater frequency of decreased hepatic, renal or cardiac function and of concomitant disease or other drug therapy.
4.7 Effects on Ability to Drive and Use Machines
Montelukast: Montelukast is not expected to affect a patient's ability to drive a car or operate machinery. However, in very rare cases, individuals have reported drowsiness or dizziness.
Levocetirizine: Comparative clinical trials have revealed no evidence that levocetirizine at the recommended dose impairs mental alertness, reactivity or the ability to drive. Nevertheless, some patients could experience somnolence, fatigue and asthenia under therapy with levocetirizine. Therefore, patients intending to drive, engage in potentially hazardous activities or operate machinery should take their response to the medicinal product into account.
4.8 Undesirable Effects
There is no data available on undesirable effects of this combination. However, side effects have been reported with individual molecules.
Montelukast
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The most common adverse reactions (incidence ≥ 5% and greater than placebo; listed in descending order of frequency) in controlled clinical trials were: upper respiratory infection, fever, headache, pharyngitis, cough, abdominal pain, diarrhea, otitis media, influenza, rhinorrhea, sinusitis, otitis.
Pediatric Patients 2 to 5 Years of Age
Asthma
Montelukast has been evaluated for safety in 573 pediatric patients 2 to 5 years of age in single- and multiple-dose studies. Cumulatively, 426 pediatric patients 2 to 5 years of age were treated with montelukast for at least 3 months, 230 for 6 months or longer, and 63 patients for one year or longer in clinical trials. In pediatric patients 2 to 5 years of age receiving montelukast, the following events occurred with a frequency ≥ 2% and more frequently than in pediatric patients who received placebo: fever, cough, abdominal pain, diarrhea, headache, rhinorrhea, sinusitis, otitis, influenza, rash, ear pain, gastroenteritis, eczema, urticaria, varicella, pneumonia, dermatitis, and conjunctivitis. Another adverse effect commonly reported in the clinical trials with montelukast in this age-group was thirst.
Pediatric Patients 6 to 23 Months of Age
Asthma
Safety and effectiveness in pediatric patients younger than 12 months of age with asthma have not been established. The safety in patients 6 to 23 months of age is supported by data from pharmacokinetic and safety and efficacy studies in asthma in this pediatric population and from adult pharmacokinetic studies.
Montelukast has been evaluated for safety in 175 pediatric patients 6 to 23 months of age with asthma. The safety profile of montelukast in a 6-week, double-blind, placebo-controlled clinical study was generally similar to the safety profile in adults and pediatric patients 2 to 14 years of age. In pediatric patients 6 to 23 months of age receiving montelukast, the following events occurred with a frequency ≥ 2% and more frequently than in pediatric patients who received placebo: upper respiratory infection, wheezing; otitis media; pharyngitis, tonsillitis, cough; and rhinitis. The frequency of less common adverse events was comparable between montelukast and placebo.
Pediatric Patients 2 to 14 Years of Age
Seasonal Allergic Rhinitis
Montelukast has been evaluated in 280 pediatric patients with seasonal allergic rhinitis 2 to 14 years of age in a 2-week, multicenter, double-blind, placebo-controlled, parallel-group safety study. Montelukast administered once daily in the evening had a safety profile similar to that of placebo. In this study, the following events occurred with a frequency ≥2% and at an incidence greater than placebo: headache, otitis media, pharyngitis, and upper respiratory infection.
The safety in patients 2 to 14 years of age with perennial allergic rhinitis is supported by the safety in patients 2 to 14 years of age with seasonal allergic rhinitis.
Pediatric Patients 6 Months to 14 Years of Age
Perennial Allergic Rhinitis
The safety in patients 2 to 14 years of age with perennial allergic rhinitis is supported by the safety in patients 2 to 14 years of age with seasonal allergic rhinitis. The safety in patients 6 to 23 months of age is supported by data from pharmacokinetic and safety and efficacy studies in asthma in this pediatric population and from adult pharmacokinetic studies.
Postmarketing Experience
The following adverse reactions have been reported in post-marketing use:
Blood and lymphatic system disorders: Increased bleeding tendency, thrombocytopenia.
Immune system disorders: Hypersensitivity reactions including anaphylaxis, hepatic eosinophilic infiltration.
Psychiatric disorders: Agitation including aggressive behavior or hostility, anxiousness, depression, disorientation, psychomotor hyperactivity dream abnormalities including nightmares, hallucinations, insomnia, irritability, memory impairment, restlessness, somnambulism, suicidal thinking and behavior (including suicide), tremor, disturbance in attention, obsessive-compulsive disorder and dysphemia. These events were reported in all age groups. However, nightmare/night terrors, aggression and behavioural changes are more frequently reported in the paediatric population.
Nervous system disorders: Drowsiness, dizziness, paraesthesia/hypoesthesia, seizures.
Respiratory, thoracic and mediastinal disorders: Epistaxis, pulmonary eosinophilia, Churg-Strauss Syndrome (CSS)
Cardiac disorders: Palpitations.
Gastro-intestinal disorders: Diarrhoea, dry mouth, dyspepsia, nausea, vomiting, pancreatitis.
Hepatobiliary disorders: Elevated levels of serum transaminases (ALT, AST), hepatitis (including cholestatic, hepatocellular, and mixed-pattern liver injury).
Skin and subcutaneous tissue disorders: Angioedema, bruising, urticaria, pruritus, erythema nodosum, erythema multiforme, Stevens-Johnson syndrome/toxic epidermal necrolysis.
Musculoskeletal and connective tissue disorders: Arthralgia, myalgia including muscle cramps
Renal and urinary disorders: Enuresis in children
General disorders and administration site conditions: Pyrexia, asthenia/fatigue, malaise, oedema.
Patients with asthma on therapy with montelukast may present with systemic eosinophilia, sometimes presenting with clinical features of vasculitis consistent with Churg-Strauss syndrome, a condition which is often treated with systemic corticosteroid therapy. These events usually, but not always, have been associated with the reduction of oral corticosteroid therapy. Physicians should be alert to eosinophilia, vasculitic rash, worsening pulmonary symptoms, cardiac complications, and/or neuropathy presenting in their patients.
The following drug-related adverse reactions in clinical studies were reported commonly (≥1/100 to <1/10) in asthmatic patients treated with montelukast and at a greater incidence than in patients treated with placebo:
|
Body System Class
|
Adult and Adolescent Patients 15 years and older
(two 12-week studies; n=795)
|
Paediatric Patients
6 to 14 years old
(one 8-week study; n=201)
(two 56-week studies; n=615)
|
|
Nervous system disorders
|
Headache
|
headache
|
|
Gastrointestinal disorders
|
abdominal pain
|
|
|
General disorders and administration site conditions
|
|
|
With prolonged treatment in clinical trials with a limited number of patients for up to 2 years for adults, and up to 12 months for paediatric patients and adolescents 6 to 14 years of age, the safety profile did not change.
Levocetirizine
Use of levocetirizine has been associated with somnolence, headache, fatigue, nasopharyngitis, dry mouth, and pharyngitis in subjects 12 years of age and older and pyrexia, somnolence, cough, and epistaxis in children 6 to 12 years of age in clinical trials. Further uncommon incidences of adverse reactions like asthenia or abdominal pain and urinary retention were observed. Additional adverse reactions of medical significance observed at a higher incidence than in placebo in adults and adolescents aged 12 years and older exposed to levocetirizine are syncope (0.2%) and weight increased (0.5%).
Adverse reactions reported in subjects 1 to 5 years of age and in 6 months to 11 months of age were pyrexia, diarrhoea, vomiting, otitis media, constipation, salivary hypersecretion, thirst, hunger, fatigue, anorexia, somnolence, psychomotor hyperactivity, sleep disorder, middle insomnia, epistaxis, pruritius, headache.
In addition to the adverse reactions reported during clinical studies and listed above, very rare cases of the following adverse drug reactions have been reported in post-marketing experience
Immune System Disorders: Hypersensitivity including anaphylaxis
Metabolism and Nutrition Disorders: Increased appetite
Psychiatric Disorders: Aggression, agitation, hallucinations, depression, insomnia, suicidal ideation.
Nervous System Disorders: Convulsion, paraesthesia, dizziness, syncope, tremor, dysguesia.
Ear and Labyrinth Disorder: Vertigo
Eyes Disorders: Visual disturbances, blurred vision
Cardiac Disorders: Palpitations, tachycardia
Respiratory, Thoracic, and Mediastinal Disorders: Dyspnoea
Gastrointestinal Disorders: Nausea, vomiting, diarrhoea
Hepatobiliary Disorders: Hepatitis
Skin and Subcutaneous Tissue Disorders: Angioneurotic oedema, fixed drug eruption, pruritus, rash, urticaria
Musculoskeletal, Connective Tissues, and Bone Disorders: Myalgia, Arthralgia
Investigations: Weight increased, abnormal liver function tests
Renal and Urinary Disorders: dysuria, urinary retention
General Disorders and Administration Site Conditions: edema
Reporting of Suspected Adverse Reactions
Reporting suspected adverse reactions after authorization of the medicinal product is important. It allows continued monitoring of the benefit/risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions via email to: medico@zorvia.com
By reporting side effects, you can help provide more information on the safety of this medicine.
4.9 Overdose
There is no data reported on the overdosage of this combination. However, overdosage has been reported with individual molecules.
Montelukast
No specific information is available on the treatment of overdosage with montelukast. In chronic asthma studies, montelukast has been administered at doses up to 200 mg/day to adult patients for 22 weeks and, in short-term studies, up to 900 mg/day to patients for approximately a week without clinically important adverse experiences.
There have been reports of acute overdosage in post-marketing experience and clinical studies of up to at least 150 mg/day with montelukast. These include reports in adults and children with a dose as high as 1000 mg. The clinical and laboratory findings observed were consistent with the safety profile in adults and pediatric patients. There were no adverse experiences in the majority of overdosage reports. The most frequently occurring adverse experiences were consistent with the safety profile of montelukast and included abdominal pain, somnolence, thirst, headache, vomiting and psychomotor hyperactivity.
In the event of overdose, it is reasonable to employ the usual supportive measures; e.g., remove unabsorbed material from the gastrointestinal tract, employ clinical monitoring, and institute supportive therapy, if required.
It is not known whether montelukast is removed by peritoneal dialysis or hemodialysis.
In chronic asthma studies, montelukast has been administered at doses up to 200 mg/day to adult patients for 22 weeks and in short-term studies, up to 900 mg/day to patients for approximately one week without clinically important adverse experiences.
There have been reports of acute overdose in post-marketing experience and clinical studies with montelukast. These include reports in adults and children with a dose as high as 1000 mg (approximately 61 mg/Kg in a 42 month old child). The clinical and laboratory findings observed were consistent with the safety profile in adults and paediatric patients.
There were no adverse experiences in the majority of overdose reports.
Symptoms of Overdose
The most frequently occurring adverse experiences were consistent with the safety profile of montelukast and included abdominal pain, somnolence, thirst, headache, vomiting, and psychomotor hyperactivity.
Management of overdose
No specific information is available on the treatment of overdose with montelukast. It is not known whether montelukast is dialysable by peritoneal- or haemo-dialysis.
Levocetirizine
Symptoms of overdose may include drowsiness in adults, and in children, initially agitation and restlessness, followed by drowsiness. There is no known specific antidote to levocetirizine. Should overdose occur consider standard measures to remove any unabsorbed drug. Gastric lavage should be considered following short-term ingestion. Levocetirizine is not effectively removed by haemodialysis.
5.0 Pharmacological Properties
Rhinam-M Syrup is a combination of montelukast and levocetirizine, the pharmacological properties of both the molecules are given separately:
5.1 Mechanism of action
The cysteinyl leukotrienes (LTC4, LTD4, LTE4) are potent inflammatory eicosanoids released from various cells including mast cells and eosinophils. These important pro-asthmatic mediators bind to cysteinyl leukotriene receptors (CysLT) found in the human airway and cause airway actions, including bronchoconstriction, mucous secretion, vascular permeability, and eosinophil recruitment.
The CysLT type-1 (CysLT1) receptor is found in the human airway (including airway smooth muscle cells and airway macrophages) and on other pro-inflammatory cells (including eosinophils and certain myeloid stem cells). CysLTs have been correlated with the pathophysiology of allergic rhinitis. In allergic rhinitis, CysLTs are released from the nasal mucosa after allergen exposure during both early- and late-phase reactions and are associated with symptoms of allergic rhinitis. Intranasal challenge with CysLTs has been shown to increase nasal airway resistance and symptoms of nasal obstruction.
Montelukast sodium is an orally active compound that binds with high affinity and selectivity to the CysLT type-1 (CysLT1) receptor. Montelukast inhibits physiologic actions of LTD4 at the CysLT1 receptor without any agonist activity. It therefore acts as a leukotriene receptor antagonist.
Levocetirizine, the (R) enantiomer of cetirizine, is a potent and selective antagonist of peripheral histamine (H1)-receptors. H1 receptors are activated by the biogenic amine histamine. Levocetirizine prevent binding of histamine to this receptors and this in turn prevent relief from the typical symptoms of allergic rhinitis. Binding studies revealed that levocetirizine has high affinity for human H1-receptors (Ki = 3.2 nmol/l). Levocetirizine has an affinity 2-fold higher than that of cetirizine (Ki = 6.3 nmol/l). Levocetirizine dissociates from H1-receptors with a half-life of 115 ± 38 min. After single administration, levocetirizine shows a receptor occupancy of 90% at 4 hours and 57% at 24 hours.
5.2 Pharmacodynamic properties
Montelukast: In patients with seasonal allergic rhinitis aged 15 years and older who received montelukast, a mean increase of 0.2% in peripheral blood eosinophil counts was noted, compared with a mean increase of 12.5% in placebo-treated patients, over the double-blind treatment periods; this reflects a mean difference of 12.3% in favor of montelukast. The relationship between these observations and the clinical benefits of montelukast noted in the clinical trials is not known.
Levocetirizine: The onset of action of levocetirizine 5 mg in controlling pollen-induced symptoms has been observed at 1 hour post drug intake in placebo-controlled trials in the model of the allergen challenge chamber. Pharmacodynamic studies in healthy volunteers demonstrate that, at half the dose levocetirizine has comparable activity to cetirizine, both in the skin and in the nose. Pharmacokinetic/pharmacodynamic relationship 5 mg levocetirizine provide a similar pattern of inhibition of histamine-induced wheal and flare than 10 mg cetirizine. As for cetirizine, the action on histamine-induced skin reactions was out of phase with the plasma concentrations. ECGs did not show relevant effects of levocetirizine on QT interval.
5.3 Pharmacokinetic properties
Montelukast: Montelukast is rapidly absorbed following oral administration. After administration of the 10 mg film-coated tablet to fasted adults, the mean peak montelukast plasma concentration (Cmax) is achieved in 3 to 4 hours (Tmax). The mean oral bioavailability is 64%. Montelukast is more than 99% bound to plasma proteins. The steady-state volume of distribution of montelukast averages 8 to 11 liters. Montelukast is extensively metabolized. Cytochrome P450 2C8 is the major enzyme in the metabolism of montelukast. The plasma clearance of montelukast averages 45 mL/min in healthy adults. Following an oral dose of radiolabeled montelukast, 86% of the radioactivity was recovered in 5-day fecal collections and <0.2% was recovered in urine. In several studies, the mean plasma half-life of montelukast ranged from 2.7 to 5.5 hours in healthy young adults.
Levocetirizine: The pharmacokinetics of levocetirizine is linear with dose and time-independent with low inter-subject variability. Levocetirizine is rapidly and extensively absorbed following oral administration. Peak plasma concentrations are achieved 0.9 hours after dosing. Steady state is achieved after 2 days. Levocetirizine is 90% bound to plasma proteins. The extent of metabolism of levocetirizine in humans is less than 14% of the dose. The plasma half-life in adults is 7.9 ± 1.9 hours. The mean apparent total body clearance is 0.63 ml/min/kg. The major route of excretion of levocetirizine and its metabolites is via the urine, accounting for a mean of 85.4% of the dose. Excretion via the faeces accounts for only 12.9% of the dose.
6.0 Nonclinical Properties
6.1 Animal Toxicology or Pharmacology
Montelukast: In animal toxicity studies, minor serum biochemical alterations in ALT, glucose, phosphorus and triglycerides were observed which were transient in nature. Montelukast was determined not to be phototoxic in mice for UVA, UVB or visible light spectra at doses up to 500 mg/kg/day (approximately >200-fold based on systemic exposure). Montelukast was neither mutagenic in in vitro and in vivo tests nor tumorigenic in rodent species.
Levocetirizine: No carcinogenicity studies have been performed with levocetirizine. However, evaluation of cetirizine carcinogenicity studies is relevant for determination of the carcinogenic potential of levocetirizine. Levocetirizine was not mutagenic in the Ames test, and not clastogenic in the human lymphocyte assay, the mouse lymphoma assay, and in vivo micronucleus test in mice.
7.0 Description
Levocetirizine Dihydrochloride
Levocetirizine Dihydrochloride is chemically 2-[2-[4-[(R)-(4-chlorophenyl) phenylmethyl]piperazin-1-yl]ethoxy]acetic acid; dihydrochloride having molecular weight of 461.8 g/mol and molecular formula is C21H27Cl3N2O3.
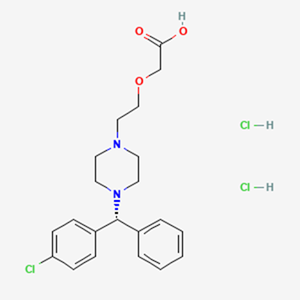
Montelukast Sodium
Montelukast Sodium is sodium;2-[1-[[(1R)-1-[3-[(E)-2-(7-chloroquinolin-2-yl)ethenyl]phenyl]-3-[2-(2-hydroxypropan-2-yl)phenyl]propyl]sulfanylmethyl] cyclopropyl] acetate having molecular weight of 608.2 g/mol and molecular formula is C35H35ClNNaO3S.
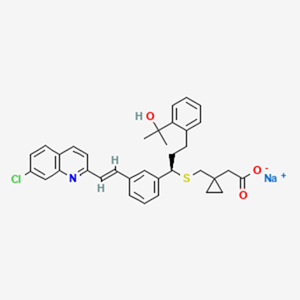
8.0 Pharmaceutical Particulars
8.1 Incompatibilities
Not applicable
8.2 Shelf-Life
Refer on pack
8.3 Packaging Information
30ml Bottle
8.4 Storage and Handling Instructions
Store below 30°C. Protect from light.
9.0 Patient Counselling Information
- RHINAM-M may cause drowsiness or fatigue. Advise patients to avoid activities requiring mental alertness (e.g., operating machinery) until they know how the medicine affects them.
- Avoid concurrent use of RHINAM-M with alcohol or other central nervous system depressants, as this may increase drowsiness and impair alertness.
- Inform patients that behavioral or mood changes (e.g., irritability, restlessness, sleep disturbances) may occur. Advise patients/caregivers to seek medical advice if such symptoms develop.
- RHINAM-M is not indicated for relief of acute asthma attacks. Advise patients to keep appropriate rescue medication available.
- Do not exceed the recommended daily dose. Advise caregivers to use a proper measuring device for accurate dosing.
- Inform the doctor before use in patients with kidney disease. RHINAM-M is contraindicated in end-stage renal disease and not recommended in patients with impaired renal function.
- Use with caution in patients predisposed to urinary retention. Discontinue RHINAM-M and seek medical advice if difficulty in passing urine occurs.
- Discontinue RHINAM-M and seek immediate medical attention if signs of hypersensitivity occur, such as rash, swelling of face or throat, or difficulty breathing.
10.0 Date of Revision
17th March 2026


