4.4 Special Warnings and Precautions for use
Diabetic ketoacidosis
Rare cases of diabetic ketoacidosis (DKA), including life-threatening and fatal cases, have been reported in patients treated with SGLT2 inhibitors, including empagliflozin. In a number of cases, the presentation of the condition was atypical with only moderately increased blood glucose values, below 14 mmol/L (250 mg/dL). It is not known if DKA is more likely to occur with higher doses of empagliflozin.
The risk of DKA must be considered in the event of non-specific symptoms such as nausea, vomiting, anorexia, abdominal pain, excessive thirst, difficulty breathing, confusion, unusual fatigue or sleepiness. Patients should be assessed for ketoacidosis immediately if these symptoms occur, regardless of blood glucose level.
In patients where DKA is suspected or diagnosed, treatment with empagliflozin should be discontinued immediately.
Treatment should be interrupted in patients who are hospitalised for major surgical procedures or acute serious medical illnesses. Monitoring of ketones is recommended in these patients. Measurement of blood ketone levels is preferred to urine. Treatment with empagliflozin may be restarted when the ketone values are normal and the patient's condition has stabilised.
Before initiating empagliflozin, factors in the patient history that may predispose to ketoacidosis should be considered.
Prolonged diabetic ketoacidosis and prolonged glucosuria have been observed with empagliflozin. Diabetic ketoacidosis may last longer after discontinuation of empagliflozin than expected from the plasma half-life. Empagliflozin-independent factors, such as insulin deficiency, might be involved in prolonged periods of diabetic ketoacidosis.
Patients who may be at higher risk of DKA include patients with a low beta-cell function reserve (e.g. type 2 diabetes patients with low C-peptide or latent autoimmune diabetes in adults (LADA) or patients with a history of pancreatitis), patients with conditions that lead to restricted food intake or severe dehydration, patients for whom insulin doses are reduced and patients with increased insulin requirements due to acute medical illness, surgery or alcohol abuse. SGLT2 inhibitors should be used with caution in these patients.
Restarting SGLT2 inhibitor treatment in patients with previous DKA while on SGLT2 inhibitor treatment is not recommended, unless another clear precipitating factor is identified and resolved.
Linectra-EF 10/25 should not be used in patients with type 1 diabetes. Data from a clinical trial program in patients with type 1 diabetes showed increased DKA occurrence with common frequency in patients treated with empagliflozin 10 mg and 25 mg as an adjunct to insulin compared to placebo.
Renal impairment
In patients with an eGFR below 60 mL/min/1.73 m2 or CrCl <60 mL/min, the daily dose of empagliflozin/linagliptin is limited to 10 mg/5 mg. Empagliflozin/linagliptin is not recommended when eGFR is below 30 mL/min/1.73 m2 or CrCl is below 30 mL/min. Empagliflozin/linagliptin should not be used in patients with ESRD or in patients on dialysis. There are insufficient data to support use in these patients.
Monitoring of renal function
Assessment of renal function is recommended as follows: prior to empagliflozin/linagliptin initiation and periodically during treatment, i.e. at least yearly; prior to initiation of any concomitant medicinal product that may have a negative impact on renal function.
Hepatic injury
Cases of hepatic injury have been reported with empagliflozin in clinical trials. A causal relationship between empagliflozin and hepatic injury has not been established.
Elevated haematocrit
Haematocrit increase was observed with empagliflozin treatment. Patients with pronounced elevations in haematocrit should be monitored and investigated for underlying haematological disease.
Chronic kidney disease
There is experience with empagliflozin for the treatment of diabetes in patients with chronic kidney disease (eGFR ≥30 mL/min/1.73 m2) both with and without albuminuria. Patients with albuminuria may benefit more from treatment with empagliflozin.
Risk for volume depletion
Based on the mode of action of SGLT2 inhibitors, osmotic diuresis accompanying therapeutic glucosuria may lead to a modest decrease in blood pressure. Therefore, caution should be exercised in patients for whom an empagliflozin-induced drop in blood pressure could pose a risk, such as patients with known cardiovascular disease, patients on anti-hypertensive therapy (e.g. thiazide and loop diuretics) with a history of hypotension or patients aged 75 years and older.
In case of conditions that may lead to fluid loss (e.g. gastrointestinal illness), careful monitoring of volume status (e.g. physical examination, blood pressure measurements, laboratory tests including haematocrit) and electrolytes is recommended for patients receiving empagliflozin. Temporary interruption of treatment with Linectra-EF 10/25 should be considered until the fluid loss is corrected.
Elderly
A higher risk of volume depletion adverse reactions was reported in patients aged 75 years and older, treated with empagliflozin, especially at 25 mg/day. Therefore, special attention should be given to their volume intake in case of co-administered medicinal products which may lead to volume depletion (e.g. diuretics, ACE inhibitors).
Urinary tract infections
In Linectra-EF 10/25 clinical trials, the incidence of urinary tract infections was overall similar between the patients treated with Linectra-EF 10/25 and the patients treated with empagliflozin or linagliptin. The frequencies were comparable to the incidence of urinary tract infections in empagliflozin clinical trials.
In a pool of placebo-controlled double-blind trials of 18 to 24 weeks duration, the overall frequency of urinary tract infection reported as adverse event was similar in patients treated with empagliflozin 25 mg and placebo and higher in patients treated with empagliflozin 10 mg. Cases of complicated urinary tract infections including pyelonephritis and urosepsis have been reported in patients treated with empagliflozin. Pyelonephritis and urosepsis were not reported from the clinical trials in patients treated with Linectra-EF 10/25. However, temporary interruption of Linectra-EF 10/25 should be considered in patients with complicated urinary tract infections.
Necrotising fasciitis of the perineum (Fournier's gangrene)
Cases of necrotising fasciitis of the perineum, (also known as Fournier's gangrene), have been reported in female and male patients taking SGLT2 inhibitors, including empagliflozin. This is a rare but serious and potentially life-threatening event that requires urgent surgical intervention and antibiotic treatment.
Patients should be advised to seek medical attention if they experience a combination of symptoms of pain, tenderness, erythema, or swelling in the genital or perineal area, with fever or malaise. Be aware that either uro-genital infection or perineal abscess may precede necrotising fasciitis. If Fournier´s gangrene is suspected, Linectra-EF 10/25 should be discontinued, and prompt treatment (including antibiotics and surgical debridement) should be instituted.
Lower limb amputations
An increase in cases of lower limb amputation (primarily of the toe) has been observed in long-term clinical trials with another SGLT2 inhibitor. It is unknown whether this constitutes a class effect. Like for all diabetic patients it is important to counsel patients on routine preventative foot-care.
Urine laboratory assessments
Due to the mechanism of action of empagliflozin, patients taking Linectra-EF 10/25 will test positive for glucose in their urine.
Interference with 1,5-anhydroglucitol (1,5-AG) assay
Monitoring glycaemic control with 1,5-AG assay is not recommended as measurements of 1,5-AG are unreliable in assessing glycaemic control in patients taking SGLT2 inhibitors. Use of alternative methods to monitor glycaemic control is advised.
Acute pancreatitis
Use of dipeptidyl peptidase-4 (DPP-4) inhibitors has been associated with a risk of developing acute pancreatitis. Acute pancreatitis has been observed in patients taking linagliptin. In a cardiovascular and renal safety trial (CARMELINA) with median observation period of 2.2 years, adjudicated acute pancreatitis was reported in 0.3% of patients treated with linagliptin and in 0.1% of patients treated with placebo. Patients should be informed of the characteristic symptoms of acute pancreatitis.
If pancreatitis is suspected, Linectra-EF 10/25 should be discontinued; if acute pancreatitis is confirmed, Linectra-EF 10/25 should not be restarted. Caution should be exercised in patients with a history of pancreatitis.
Bullous pemphigoid
Bullous pemphigoid has been observed in patients taking linagliptin. In the CARMELINA trial, bullous pemphigoid was reported in 0.2% of patients on treatment with linagliptin and in no patient on placebo. If bullous pemphigoid is suspected, Linectra-EF 10/25 should be discontinued.
Use with medicinal products known to cause hypoglycaemia
Empagliflozin and linagliptin as single agents showed an incidence of hypoglycaemia comparable to placebo when used alone or in combination with other antidiabetics not known to cause hypoglycaemia (e.g. metformin, thiazolidinediones). When used in combination with antidiabetics known to cause hypoglycaemia (e.g. sulphonylureas and/or insulin), the incidence of hypoglycaemia of both agents was increased.
There are no data about the hypoglycaemic risk of Linectra-EF 10/25 when used with insulin and/or sulphonylurea. However, caution is advised when Linectra-EF 10/25 is used in combination with antidiabetics. A dose reduction of the sulphonylurea or insulin may be considered.
4.5 Drug Interactions
Table 1: Clinically relevant interactions with Linectra-EF 10/25
|
Diuretics
|
|
Clinical Impact
|
Coadministration of empagliflozin with diuretics resulted in increased urine volume and frequency of voids, which might enhance the potential for volume depletion.
|
|
Intervention
|
Before initiating Linectra-EF 10/25, assess volume status and renal function. In patients with volume depletion, correct this condition before initiating Linectra-EF 10/25. Monitor for signs and symptoms of volume depletion, and renal function after initiating therapy
|
|
Insulin or Insulin Secretagogues
|
|
Clinical Impact
|
The risk of hypoglycemia is increased when Linectra-EF 10/25is used in combination with an insulin secretagogue (e.g., sulfonylurea) or insulin.
|
|
Intervention
|
Coadministration of Linectra-EF 10/25 with an insulin secretagogue (e.g., sulfonylurea) or insulin may require lower dosages of the insulin secretagogue or insulin to reduce the risk of hypoglycemia
|
|
Lithium
|
|
Clinical Impact
|
Concomitant use of an SGLT2 inhibitor with lithium may decrease serum lithium concentrations.
|
|
Intervention
|
Monitor serum lithium concentration more frequently during Linectra-EF 10/25 initiation and dosage changes.
|
|
Inducers of P-glycoprotein or CYP3A4 Enzymes
|
|
Clinical Impact
|
Rifampin decreased linagliptin exposure, suggesting that the efficacy of linagliptin may be reduced when administered in combination with a strong P-gp or CYP3A4 inducer.
|
|
Intervention
|
Use of alternative treatments is strongly recommended when linagliptin is to be administered with a strong P-gp or CYP3A4 inducer
|
|
Positive Urine Glucose Test
|
|
Clinical Impact
|
SGLT2 inhibitors increase urinary glucose excretion and will lead to positive urine glucose tests.
|
|
Intervention
|
Monitoring glycemic control with urine glucose tests is not recommended in patients taking SGLT2 inhibitors. Use alternative methods to monitor glycemic control
|
|
Interference with 1,5-anhydroglucitol (1,5-AG) Assay
|
|
Clinical Impact
|
Measurements of 1,5-AG are unreliable in assessing glycemic control in patients taking SGLT2 inhibitors.
|
|
Intervention
|
Monitoring glycemic control with 1,5-AG assay is not recommended. Use alternative methods to monitor glycemic control
|
5.0 Pharmacological Properties
5.1 Mechanism of Action
Linectra-EF 10/25 contains: empagliflozin, a SGLT2 inhibitor, and linagliptin, a DPP-4 inhibitor.
Empagliflozin
Empagliflozin is an inhibitor of SGLT2, the predominant transporter responsible for reabsorption of glucose from the glomerular filtrate back into the circulation. By inhibiting SGLT2, empagliflozin reduces renal reabsorption of filtered glucose and lowers the renal threshold for glucose and thereby increases urinary glucose excretion.
Linagliptin
Linagliptin is an inhibitor of DPP-4, an enzyme that degrades the incretin hormones glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP). Thus, linagliptin increases the concentrations of active incretin hormones, stimulating the release of insulin in a glucose-dependent manner and decreasing the levels of glucagon in the circulation. Both incretin hormones are involved in the physiological regulation of glucose homeostasis. Incretin hormones are secreted at a low basal level throughout the day and levels rise immediately after meal intake. GLP-1 and GIP increase insulin biosynthesis and secretion from pancreatic beta cells in the presence of normal and elevated blood glucose levels. Furthermore, GLP-1 also reduces glucagon secretion from pancreatic alpha cells, resulting in a reduction in hepatic glucose output.
5.2 Pharmacodynamic Properties
Empagliflozin
Urinary Glucose Excretion: In patients with type 2 diabetes mellitus, urinary glucose excretion increased immediately following a dose of empagliflozin and was maintained at the end of a 4-week treatment period averaging at approximately 64 grams per day with 10 mg empagliflozin and 78 grams per day with 25 mg empagliflozin once daily. Data from single oral doses of empagliflozin in healthy subjects indicate that, on average, the elevation in urinary glucose excretion approaches baseline by about 3 days for the 10 mg and 25 mg doses.
Urinary Volume: In a 5-day study, mean 24-hour urine volume increase from baseline was 341 mL on Day 1 and 135 mL on Day 5 of empagliflozin 25 mg once daily treatment.
Cardiac Electrophysiology: In a randomized, placebo-controlled, active-comparator, crossover study, 30 healthy subjects were administered a single oral dose of empagliflozin 25 mg, empagliflozin 200 mg (8 times the maximum recommended dose), moxifloxacin, and placebo. No increase in QTc was observed with either 25 mg or 200 mg empagliflozin.
Linagliptin
Linagliptin binds to DPP-4 in a reversible manner and increases the concentrations of incretin hormones. Linagliptin glucose-dependently increases insulin secretion and lowers glucagon secretion, thus resulting in a better regulation of the glucose homeostasis. Linagliptin binds selectively to DPP-4 and selectively inhibits DPP-4, but not DPP-8 or DPP-9 activity in vitro at concentrations approximating therapeutic exposures.
Cardiac Electrophysiology: In a randomized, placebo-controlled, active-comparator, 4-way crossover study, 36 healthy subjects were administered a single oral dose of linagliptin 5 mg, linagliptin 100 mg (20 times the recommended dose), moxifloxacin, and placebo. No increase in QTc was observed with either the recommended dose of 5 mg or the 100 mg dose. At the 100 mg dose, peak linagliptin plasma concentrations were approximately 38-fold higher than the peak concentrations following a 5-mg dose.
5.3 Pharmacokinetic Properties
Linectra-EF 10/25
Administration of the fixed-dose combination with food resulted in no change in overall exposure of empagliflozin or linagliptin; however, the peak exposure was decreased 39% and 32% for empagliflozin and linagliptin, respectively. These changes are not likely to be clinically significant.
Empagliflozin
The pharmacokinetics of empagliflozin has been characterized in healthy volunteers and patients with type 2 diabetes mellitus and no clinically relevant differences were noted between the two populations. The steady-state mean plasma AUC and Cmax were 1,870 nmol.h/L and 259 nmol/L, respectively, with 10 mg empagliflozin once daily treatment, and 4,740 nmol.h/L and 687 nmol/L, respectively, with 25 mg empagliflozin once daily treatment. Systemic exposure of empagliflozin increased in a dose-proportional manner in the therapeutic dose range. Empagliflozin does not appear to have time-dependent pharmacokinetic characteristics. Following once-daily dosing, up to 22% accumulation, with respect to plasma AUC, was observed at steady-state.
Absorption: After oral administration, peak plasma concentrations of empagliflozin were reached at 1.5 hours post-dose. Administration of 25 mg empagliflozin after intake of a high-fat and high-calorie meal resulted in slightly lower exposure; AUC decreased by approximately 16% and Cmax decreased by approximately 37%, compared to fasted condition. The observed effect of food on empagliflozin pharmacokinetics was not considered clinically relevant and empagliflozin may be administered with or without food.
Distribution: The apparent steady-state volume of distribution was estimated to be 73.8 L based on a population pharmacokinetic analysis. Following administration of an oral [14C]-empagliflozin solution to healthy subjects, the red blood cell partitioning was approximately 36.8% and plasma protein binding was 86.2%.
Elimination: The apparent terminal elimination half-life of empagliflozin was estimated to be 12.4 h and apparent oral clearance was 10.6 L/h based on the population pharmacokinetic analysis.
Metabolism: No major metabolites of empagliflozin were detected in human plasma and the most abundant metabolites were three glucuronide conjugates (2-O-, 3-O-, and 6-O-glucuronide). Systemic exposure of each metabolite was less than 10% of total drug-related material. In vitro studies suggested that the primary route of metabolism of empagliflozin in humans is glucuronidation by the uridine 5'-diphospho-glucuronosyltransferases UGT2B7, UGT1A3, UGT1A8, and UGT1A9.
Excretion: Following administration of an oral [14C]-empagliflozin solution to healthy subjects, approximately 95.6% of the drug-related radioactivity was eliminated in feces (41.2%) or urine (54.4%). The majority of drug-related radioactivity recovered in feces was unchanged parent drug and approximately half of drug-related radioactivity excreted in urine was unchanged parent drug.
Linagliptin
Absorption: The absolute bioavailability of linagliptin is approximately 30%. A high-fat meal reduced Cmax by 15% and increased AUC by 4%; this effect is not clinically relevant. Linagliptin may be administered with or without food.
Distribution: The mean apparent volume of distribution at steady-state following a single intravenous dose of linagliptin 5 mg to healthy subjects is approximately 1,110 L, indicating that linagliptin extensively distributes to the tissues. Plasma protein binding of linagliptin is concentration-dependent, decreasing from about 99% at 1 nmol/L to 75% to 89% at ≥30 nmol/L, reflecting saturation of binding to DPP-4 with increasing concentration of linagliptin. At high concentrations, where DPP-4 is fully saturated, 70% to 80% of linagliptin remains bound to plasma proteins and 20% to 30% is unbound in plasma. Plasma binding is not altered in patients with renal or hepatic impairment.
Elimination: Linagliptin has a terminal half-life of about 200 hours at steady state, though the accumulation half-life is about 11 hours. Renal clearance at steady state was approximately 70 mL/min.
Metabolism: Following oral administration, the majority (about 90%) of linagliptin is excreted unchanged, indicating that metabolism represents a minor elimination pathway. A small fraction of absorbed linagliptin is metabolized to a pharmacologically inactive metabolite, which shows a steady-state exposure of 13.3% relative to linagliptin.
Excretion: Following administration of an oral [14C]-linagliptin dose to healthy subjects, approximately 85% of the administered radioactivity was eliminated via the enterohepatic system (80%) or urine (5%) within 4 days of dosing.
6.0 Nonclinical Properties
6.1 Animal Toxicology or Pharmacology
No carcinogenicity, mutagenicity, or impairment of fertility studies have been conducted with the combination of empagliflozin and linagliptin.
Empagliflozin
Carcinogenesis was evaluated in 2-year studies conducted in CD-1 mice and Wistar rats. Empagliflozin did not increase the incidence of tumours in female rats dosed at 100, 300, or 700 mg/kg/day (up to 72 times the exposure from the maximum clinical dose of 25 mg). In male rats, hemangiomas of the mesenteric lymph node were increased significantly at 700 mg/kg/day or approximately 42 times the exposure from a 25 mg clinical dose. Empagliflozin did not increase the incidence of tumors in female mice dosed at 100, 300, or 1,000 mg/kg/day (up to 62 times the exposure from a 25 mg clinical dose). Renal tubule adenomas and carcinomas were observed in male mice at 1,000 mg/kg/day, which is approximately 45 times the exposure of the maximum clinical dose of 25 mg. These tumors may be associated with a metabolic pathway predominantly present in the male mouse kidney.
Empagliflozin was not mutagenic or clastogenic with or without metabolic activation in the in vitro Ames bacterial mutagenicity assay, the in vitro L5178Y tk+/-mouse lymphoma cell assay, and an in vivo micronucleus assay in rats.
Empagliflozin had no effects on mating, fertility or early embryonic development in treated male or female rats up to the high dose of 700 mg/kg/day (approximately 155 times the 25 mg clinical dose in males and females, respectively).
Linagliptin
Linagliptin did not increase the incidence of tumors in male and female rats in a 2-year study at doses of 6, 18, and 60 mg/kg. The highest dose of 60 mg/kg is approximately 418 times the clinical dose of 5 mg/day based on AUC exposure. Linagliptin did not increase the incidence of tumors in mice in a 2-year study at doses up to 80 mg/kg (males) and 25 mg/kg (females), or approximately 35- and 270-times the clinical dose based on AUC exposure. Higher doses of linagliptin in female mice (80 mg/kg) increased the incidence of lymphoma at approximately 215-times the clinical dose based on AUC exposure.
Linagliptin was not mutagenic or clastogenic with or without metabolic activation in the Ames bacterial mutagenicity assay, a chromosomal aberration test in human lymphocytes, and an in vivo micronucleus assay.
In fertility studies in rats, linagliptin had no adverse effects on early embryonic development, mating, fertility, or bearing live young up to the highest dose of 240 mg/kg (approximately 943-times the clinical dose based on AUC exposure).
7.0 Description
Linectra-EF 10/25 tablets for oral use contain Empagliflozin and linagliptin.
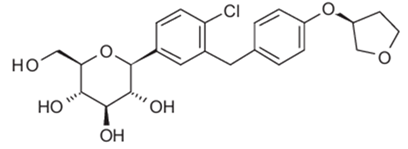
Empagliflozin
Empagliflozin is an inhibitor of the SGLT2.
Chemical name: D-Glucitol,1,5-anhydro-1-C-[4-chloro-3-[[4-[[(3S)-tetrahydro-3-furanyl]oxy]phenyl]methyl]phenyl]-, (1S).
Molecular formula: C23H27ClO7
Molecular weight: 450.91
Linagliptin
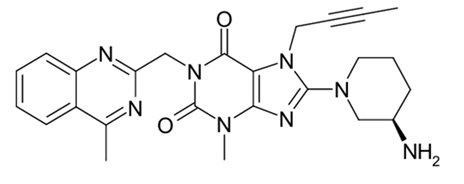
Linagliptin is an inhibitor of the dipeptidyl peptidase-4 (DPP-4) enzyme
Chemical name: 1H-Purine-2,6-dione, 8-[(3R)-3-amino-1-piperidinyl]-7-(2-butyn-1-yl)-3,7-dihydro-3-methyl-1-[(4-methyl-2-quinazolinyl)methyl]-
Molecular formula: C25H28N8O2
Molecular weight: 472.54 g/mol.
8.0 Pharmaceutical Particulars
8.1 Incompatibilities
None.
8.2 Shelf-Life
Refer on pack.
8.3 Packaging Information
As per carton.
8.4 Storage and Handling Instructions
Keep out of reach of children.
Store below 30°C in a dry place. Protect from light.
9.0 Patient Counselling Information
Diabetic Ketoacidosis in Patients with Type 1 Diabetes Mellitus and Other Ketoacidosis
Inform patients that Linectra-EF 10/25 can cause potentially fatal ketoacidosis and that type 2 diabetes mellitus and pancreatic disorders (e.g., history of pancreatitis or pancreatic surgery) are risk factors. Educate all patients on precipitating factors (such as insulin dose reduction or missed insulin doses, infection, reduced caloric intake, ketogenic diet, surgery, dehydration, and alcohol abuse) and symptoms of ketoacidosis (including nausea, vomiting, abdominal pain, tiredness, and laboured breathing). Inform patients that blood glucose may be normal even in the presence of ketoacidosis. Advise patients that they may be asked to monitor ketones. If symptoms of ketoacidosis occur, instruct patients to discontinue Linectra-EF 10/25 and seek medical attention immediately.
Pancreatitis
Inform patients that acute pancreatitis has been reported during use of linagliptin. Inform patients that persistent severe abdominal pain, sometimes radiating to the back, which may or may not be accompanied by vomiting, is the hallmark symptom of acute pancreatitis. Instruct patients to discontinue Linectra-EF 10/25 promptly and contact their healthcare provider if persistent severe abdominal pain occurs.
Volume Depletion
Inform patients that symptomatic hypotension may occur with Linectra-EF 10/25 and advise them to contact their healthcare provider if they experience such symptoms. Inform patients that dehydration may increase the risk for hypotension, and to maintain adequate fluid intake.
Genitourinary Infections, including Urosepsis, Pyelonephritis, Necrotizing Fasciitis of the Perineum (Fournier's Gangrene), and Genital Mycotic Infections
Counsel patients that genitourinary infections may occur when taking empagliflozin, a component of Linectra-EF 10/25, and may become serious. Educate them on the symptoms and advise them to seek medical advice if symptoms occur. Specifically, advise patients to promptly seek medical attention if they develop pain or tenderness, redness, or swelling of the genitals or the area from the genitals back to the rectum, along with a fever above 100.4°F or malaise.
Hypoglycaemia with Concomitant Use with Insulin and Insulin Secretagogues
Inform patients that the risk of hypoglycemia is increased when Linectra-EF 10/25 is used in combination with an insulin secretagogue (e.g., sulfonylurea) or insulin.
Lower Limb Amputation
Counsel patients about the importance of routine preventative foot care. Instruct patients to monitor for new pain or tenderness, sores or ulcers, or infections involving the leg or foot and to seek medical advice immediately if such signs or symptoms develop.
Hypersensitivity Reactions
Inform patients that serious allergic reactions, such as anaphylaxis, angioedema, and exfoliative skin conditions, have been reported during use of linagliptin or empagliflozin, components of Linectra-EF 10/25. If symptoms of allergic reactions (such as rash, skin flaking or peeling, urticaria, swelling of the skin, or swelling of the face, lips, tongue, and throat that may cause difficulty in breathing or swallowing) occur, patients must stop taking Linectra-EF 10/25 and seek medical advice promptly.
Severe and Disabling Arthralgia
Inform patients that severe and disabling joint pain may occur with this class of drugs. The time to onset of symptoms can range from one day to years. Instruct patients to seek medical advice if severe joint pain occurs.
Bullous Pemphigoid
Inform patients that bullous pemphigoid has been reported during use of linagliptin. Instruct patients to seek medical advice if blisters or erosions occur.
Heart Failure
Inform patients of the signs and symptoms of heart failure. Before initiating Linectra-EF 10/25, patients should be asked about a history of heart failure or other risk factors for heart failure including moderate to severe renal impairment. Instruct patients to contact their healthcare provider as soon as possible if they experience symptoms of heart failure, including increasing shortness of breath, rapid increase in weight or swelling of the feet.
Laboratory Tests
Inform patients that elevated glucose in urinalysis is expected when taking Linectra-EF 10/25.
Pregnancy
Advise pregnant patients, and patients of reproductive potential, of the potential risk to a fetus with treatment with Linectra-EF 10/25. Instruct patients to report pregnancies to their healthcare provider as soon as possible.
Lactation
Advise patients that breastfeeding is not recommended during treatment with Linectra-EF 10/25.
Missed Dose
Instruct patients to take Linectra-EF 10/25 only as prescribed. If a dose is missed, it should be taken as soon as the patient remembers. Advise patients not to double their next dose.


